Paired blood cultures more sensitive than single for candidaemia
Guidelines (CLSI / UK SMI / ESCMID) often recommend taking 2 or 3 sets of blood cultures from different peripheral body sites, to maximise the sensitivity and give a better likelihood of isolating the causative agent for identification and susceptibility testing. However, this is not always achieved in practice for reasons of cost or feasibility (e.g. paediatric patients).
- Read the full UK Standards for Microbiology Investigations B 37: Investigation of blood cultures (for organisms other than Mycobacterium species), updated Aug 2018
This is supported by results published recently by Dr Bansidar Tarai and colleagues, who analysed data from the Max Super Speciality Hospital in New Delhi (India). 112,570 blood culture sets were processed over a 5 year period (44% paired sets, 56% single sets) using the BacT/ALERT® system (for aerobic growth) and VITEK® 2 Compact system (for identification). The overall positivity rate (bacteria and Candida combined) among inpatients was higher for paired blood cultures (10.9%) than for single cultures (6.5%), but the proportion of contaminants was not substantially higher (0.9% versus 0.7%) (Fig 1). Contaminants were primarily Staphylococcus spp. Paired aerobic blood cultures were more often positive than single cultures for most species of Candida (Fig 2).
- Read the full paper: Tarai et al (2018) Paired blood cultures increase the sensitivity for detecting pathogens in both inpatients and outpatients. Eur J Clin Microbiol Infect Dis. 2018 Mar;37(3):435-441
What can a clinician do?
- Draw plenty of blood (20-30 ml for adults, i.e. 10 ml per bottle): there is around a 3% increase in yield for each extra ml of blood (UK SMI)
- Take samples before starting antimicrobial therapy, or just before a dose is administered
- Take blood samples as soon as possible after a spike of fever
- Test daily if candidaemia is suspected
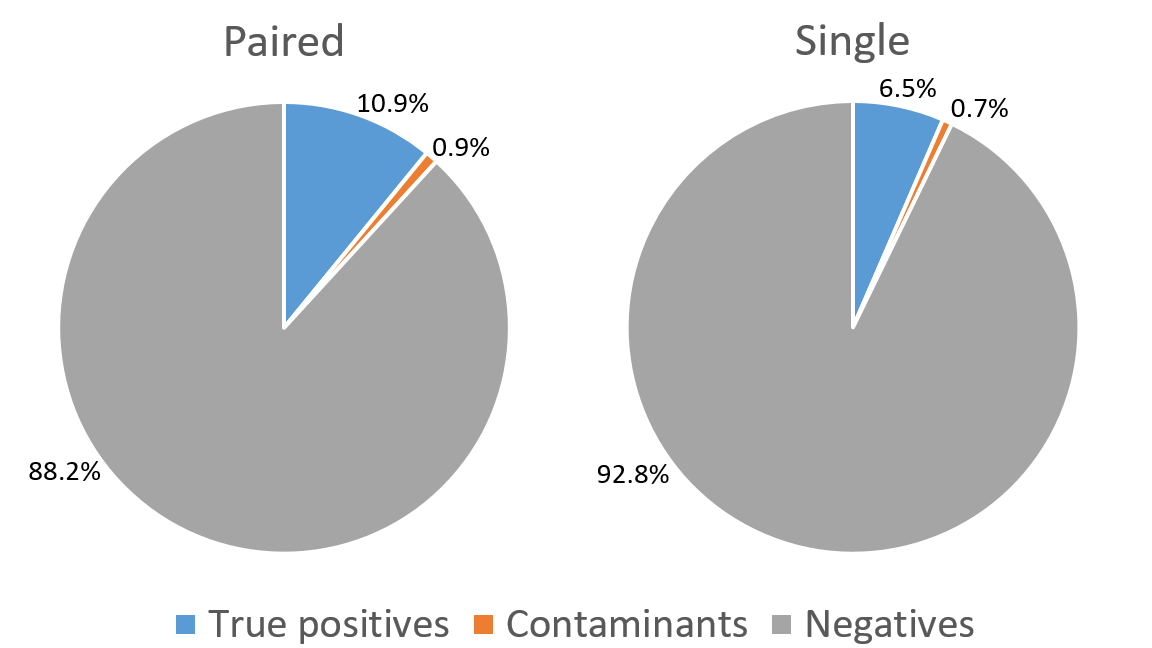
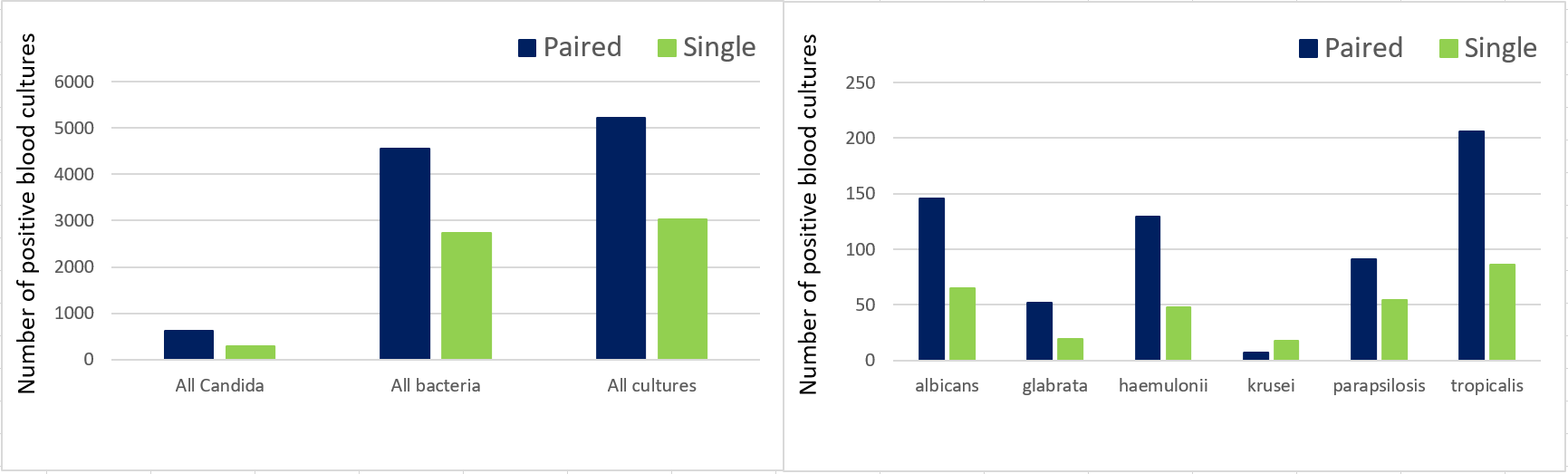
(Figures redrawn from Tarai et al 2018, data from hospital inpatients only shown)